Items filtered by date: April 2022
Where Heel Pain Occurs May Provide Clues to Its Cause

Heel pain can be caused by a variety of conditions, with the most common being plantar fasciitis: an inflammation of the plantar fasciitis tissue on the bottom of the foot. Identifying where the pain is specifically located in the heel can sometimes help your podiatrist diagnose your condition. For instance, plantar fasciitis usually causes pain in the bottom/middle of the heel which is at its worst when you first wake up in the morning. Other conditions, such as heel stress fractures, nerve issues, or heel pad atrophy can also cause pain on the bottom of the heel. Pain in the back of the heel may be caused by problems with your Achilles tendon, which connects the heel bone to the calf muscles. These conditions include Achilles tendinopathy/tendinitis, which is usually an overuse injury to the tendon, Haglund’s deformity, which produces a bump at the back of the heel due to shoes exerting pressure on the tendon, and Sever’s disease, which is due to stress on the heel’s growth plate in growing children. Pain in the middle of the heel can sometimes be caused by an entrapped nerve in the ankle (tarsal tunnel syndrome). Sinus tarsi syndrome, typically due to flat feet or following an ankle sprain, can cause pain in the middle/side portion of the heel. Any type of heel pain should be examined by a podiatrist to receive proper diagnosis and treatment.
Many people suffer from bouts of heel pain. For more information, contact Dr. Odin De Los Reyes of Connecticut. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our offices located in Southbury and Farmington, CT . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
The Pandemic and Running Injuries
 The pandemic prevented many people from engaging in workouts in the gym. Research has shown it may help to begin running slowly on the treadmill before venturing outside on pavement or trails. This may help to prevent running injuries and may be a result of the body warming up to run again. It is suggested that when people resume running outside, the speed and mileage are gradually increased. Covid 19 isolation may have changed people’s running habits, and this may have happened from anxiety, remote work, and schooling. They may have had less time to run than they previously had and may compensate for that by running harder and longer. Wearing shoes that fit correctly and being aware of your running regime is instrumental in preventing running injuries. If you would like information about how running injuries can affect the feet, please consult with a podiatrist, who can recommend additional methods on how to prevent them.
The pandemic prevented many people from engaging in workouts in the gym. Research has shown it may help to begin running slowly on the treadmill before venturing outside on pavement or trails. This may help to prevent running injuries and may be a result of the body warming up to run again. It is suggested that when people resume running outside, the speed and mileage are gradually increased. Covid 19 isolation may have changed people’s running habits, and this may have happened from anxiety, remote work, and schooling. They may have had less time to run than they previously had and may compensate for that by running harder and longer. Wearing shoes that fit correctly and being aware of your running regime is instrumental in preventing running injuries. If you would like information about how running injuries can affect the feet, please consult with a podiatrist, who can recommend additional methods on how to prevent them.
All runners should take extra precaution when trying to avoid injury. If you have any concerns about your feet, contact Dr. Odin De Los Reyes of Connecticut. Our doctor will treat your foot and ankle needs.
How to Prevent Running Injuries
There are a lot of mistakes a runner can make prior to a workout that can induce injury. A lot of athletes tend to overstretch before running, instead of saving those workouts for a post-run routine. Deep lunges and hand-to-toe hamstring pulls should be performed after a workout instead of during a warmup. Another common mistake is jumping into an intense routine before your body is physically prepared for it. You should try to ease your way into long-distance running instead of forcing yourself to rush into it.
More Tips for Preventing Injury
- Incorporate Strength Training into Workouts - This will help improve the body’s overall athleticism
- Improve and Maintain Your Flexibility – Stretching everyday will help improve overall performance
- “Warm Up” Before Running and “Cool Down” Afterward – A warm up of 5-10 minutes helps get rid of lactic acid in the muscles and prevents delayed muscle soreness
- Cross-Training is Crucial
- Wear Proper Running Shoes
- Have a Formal Gait Analysis – Poor biomechanics can easily cause injury
If you have any questions, please feel free to contact our offices located in Southbury and Farmington, CT . We offer the newest diagnostic and treatment technologies for all your foot care needs.
It's Time for Beautiful Feet
Do I Have Athlete’s Foot?
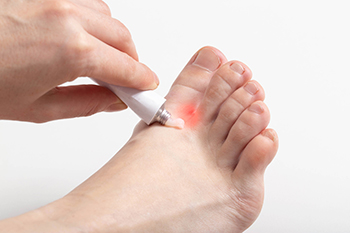 Athlete’s foot presents itself as skin patches and skin breaks, especially between the toes, but possibly also on the bottom of the feet and toenails. This skin affliction can become red, itchy, and moist. Blisters may also form on the feet. In the worst cases, feet might ooze pus and smell foul. Athlete’s foot is most often developed from walking in areas that are damp and prone to fungus, such as locker rooms or swimming pool changing areas. While this condition is not serious, it can spread to other areas of the body and other people. If one suspects they have athlete’s foot they should use care and take precautions to prevent its spread, practice good foot hygiene, apply an antifungal cream to the affected area, and allow the feet to breathe as much as possible since shoes and socks allow for the ideal breeding ground of dampness, darkness, and warmth to proliferate. If left untreated, Athlete’s foot can become painful and interfere with activity. A podiatrist should be consulted if no improvement is seen after two weeks, if the infection appears severe, or if underlying conditions such as diabetes or circulation problems exist.
Athlete’s foot presents itself as skin patches and skin breaks, especially between the toes, but possibly also on the bottom of the feet and toenails. This skin affliction can become red, itchy, and moist. Blisters may also form on the feet. In the worst cases, feet might ooze pus and smell foul. Athlete’s foot is most often developed from walking in areas that are damp and prone to fungus, such as locker rooms or swimming pool changing areas. While this condition is not serious, it can spread to other areas of the body and other people. If one suspects they have athlete’s foot they should use care and take precautions to prevent its spread, practice good foot hygiene, apply an antifungal cream to the affected area, and allow the feet to breathe as much as possible since shoes and socks allow for the ideal breeding ground of dampness, darkness, and warmth to proliferate. If left untreated, Athlete’s foot can become painful and interfere with activity. A podiatrist should be consulted if no improvement is seen after two weeks, if the infection appears severe, or if underlying conditions such as diabetes or circulation problems exist.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact Dr. Odin De Los Reyes from Connecticut. Our doctor will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
- Hydrate your feet by using lotion
- Exfoliate
- Buff off nails
- Use of anti-fungal products
- Examine your feet and visit your doctor if any suspicious blisters or cuts develop
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact our offices located in Southbury and Farmington, CT . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Maintaining Strength May Help to Prevent Falling
 Research has indicated that falling is the leading cause of many injuries in the United States. The feet are often affected when a fall has occurred, which may result in broken toes or a broken foot. The fear of falling can cause seniors to limit completing daily activities. This behavior may cause the patient to become weakened, and falling may happen more often. Falls may be prevented by becoming stronger, and this is often done through participating in an exercise program. There are measures that can be implemented in the household that may help to prevent falling as well. These can include installing grab bars in the toilet and shower area, and improving lighting in the living areas. Many people find it helpful to use a bathmat, in addition to removing worn rugs from the steps. If you would like more information about how falling can affect the feet, and how to prevent it, please consult with a podiatrist.
Research has indicated that falling is the leading cause of many injuries in the United States. The feet are often affected when a fall has occurred, which may result in broken toes or a broken foot. The fear of falling can cause seniors to limit completing daily activities. This behavior may cause the patient to become weakened, and falling may happen more often. Falls may be prevented by becoming stronger, and this is often done through participating in an exercise program. There are measures that can be implemented in the household that may help to prevent falling as well. These can include installing grab bars in the toilet and shower area, and improving lighting in the living areas. Many people find it helpful to use a bathmat, in addition to removing worn rugs from the steps. If you would like more information about how falling can affect the feet, and how to prevent it, please consult with a podiatrist.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Dr. Odin De Los Reyes from Connecticut. Our doctor will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
- Enrolling in strength and balance exercise program to increase balance and strength
- Periodically having your sight and hearing checked
- Discuss any medications you have with a doctor to see if it increases the risk of falling
- Clearing the house of falling hazards and installing devices like grab bars and railings
- Utilizing a walker or cane
- Wearing shoes that provide good support and cushioning
- Talking to family members about falling and increasing awareness
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our offices located in Southbury and Farmington, CT . We offer the newest diagnostic and treatment technologies for all your foot care needs.