Proper Footwear for Restaurant Workers

Proper footwear is essential for restaurant workers as a way of maintaining health and comfort throughout long shifts. These jobs often involve extended periods of standing and walking on hard surfaces, which can lead to foot, leg, and back pain if the right shoes are not worn. Proper footwear provides necessary support, cushioning, and stability, helping to absorb shock and reduce the risk of injuries such as sprains or stress fractures. Shoes with slip-resistant soles also enhance safety by preventing slips and falls in potentially hazardous kitchen environments. Additionally, wearing well-fitted, supportive shoes can help alleviate common issues like plantar fasciitis and bunions. Investing in high-quality, ergonomic footwear ensures that restaurant workers remain comfortable and protected. If you work in the restaurant industry and have endured a foot injury or have developed chronic foot pain, it is suggested that you speak with a podiatrist. This type of doctor can offer effective treatment options, in addition to guiding you toward wearing appropriate footwear for the job.
While working on the feet, it is important to take the proper care of them. For more information about working on your feet, contact Dr. Odin De Los Reyes from Connecticut. Our doctor will treat your foot and ankle needs.
Working on Your Feet
Standing on your feet for long periods of time can cause stress and pain in your feet. Your whole body may experience change in terms of posture, back pain, bunions, callouses and or plantar warts. There are ways to avoid these conditions with proper foot care, smart choices and correct posture.
Positive Changes
Negative heeled shoe – Choosing this shoe type places the heel slightly lower than the ball of the foot. These are great for overall foot health. Find shoes that fit you correctly.
Go barefoot – Our feet were not designed to be enclosed for all hours of the day. Try to periodically expose your feet to air.
Eliminate Pain
Foot Exercises – Performing simple exercises, incorporating yoga and doing stretches are beneficial. This will allow increased blood flow to the area and muscles of the foot.
Achilles tendon – Stretching the foot out flat on the floor will relax the calf muscles and tendon. These exercises can be performed almost anywhere. Make sure you add these exercises to your daily regimen.
With a little bit of this information and knowing more about foot health, you will notice changes. Foot stretches and proper footwear will help with pain and prevent further issues.
If you have any questions please feel free to contact our offices located in Southbury and Farmington, CT . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Working on Your Feet
Foot care is important regardless of your profession, but those who work on their feet must pay special attention. Bunions, calluses, blisters, and plantar warts are just a few of the many conditions that can arise after standing all day. While painful at their worst, these conditions can easily be avoided with the right foot care. This includes both appropriate footwear and proper posture—important elements that affect the health of your feet.
Choosing appropriate footwear means choosing a shoe that has a negative heel. This means that the heel is slightly lower than the ball of your foot, which places less of a strain. If you have a profession that requires you to be on your feet all day, investing in a pair of high-quality shoes is pertinent. High-quality shoes can be purchased from a respected manufacturer that emphasizes foot care and foot health.
Despite the regularity of wearing shoes, the feet are naturally not designed to be enclosed. Regular “barefoot” time for your feet can be beneficial for foot health. Among other methods, allowing your feet to breathe can help alleviate the pain and pressure your feet may be experiencing from being on your feet all day.
Simple foot exercises and yoga positions can help improve both the health and function of your feet. Active foot exercises that create movement will stimulate your foot’s blood flow and circulation, and yoga positions that place your feet flat onto the floor will stretch out their muscles. Yoga is particularly beneficial for your Achilles tendon and calf muscles, which are areas that can become especially problematic if not taken care of. Foot exercises and yoga positions can be easily performed every day at virtually any location and any time; whether it is at the office, at the gym, or at home right before you go to bed. Simple stretching can increase your foot health by miles.
The foot pain you experience after lengthy hours working on your feet may seem inevitable and unavoidable; in reality, however, that is not the case. Wearing proper footwear and performing simple foot exercises and stretches can help ease foot pain and allow you to truly avoid frustrating foot problems.
Your feet can easily be kept healthy with some education and a little effort. Pain that begins at the feet can eventually affect the whole body. Begin taking care of your feet now!
Plantar Fasciitis Relief
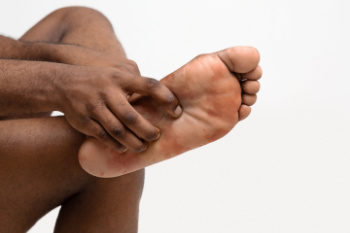 Plantar fasciitis is a common cause of heel pain, resulting from inflammation of the plantar fascia, which is a thick band of tissue connecting the heel bone to the toes. This condition often develops due to repetitive strain or overuse, common in runners, people who stand for long periods, or those with high arches or flat feet. Symptoms can include sharp, stabbing pain in the heel, especially noticeable with the first steps in the morning or after prolonged sitting. The pain typically decreases with movement but may return after extended activity. Contributing factors include wearing unsupportive footwear, obesity, and having tight calf muscles. Treatment focuses on relieving inflammation and pain. Common approaches include rest, stretching exercises, and using orthotic inserts to support the arch. Nonsteroidal anti-inflammatory drugs can also help to reduce pain and swelling. In persistent cases, corticosteroid injections or surgery may be considered. If you have heel pain, it is suggested that you visit a podiatrist for a proper diagnosis and tailored treatment plan.
Plantar fasciitis is a common cause of heel pain, resulting from inflammation of the plantar fascia, which is a thick band of tissue connecting the heel bone to the toes. This condition often develops due to repetitive strain or overuse, common in runners, people who stand for long periods, or those with high arches or flat feet. Symptoms can include sharp, stabbing pain in the heel, especially noticeable with the first steps in the morning or after prolonged sitting. The pain typically decreases with movement but may return after extended activity. Contributing factors include wearing unsupportive footwear, obesity, and having tight calf muscles. Treatment focuses on relieving inflammation and pain. Common approaches include rest, stretching exercises, and using orthotic inserts to support the arch. Nonsteroidal anti-inflammatory drugs can also help to reduce pain and swelling. In persistent cases, corticosteroid injections or surgery may be considered. If you have heel pain, it is suggested that you visit a podiatrist for a proper diagnosis and tailored treatment plan.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. Odin De Los Reyes from Connecticut. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact our offices located in Southbury and Farmington, CT . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
Facts About Ankle Replacement Surgery
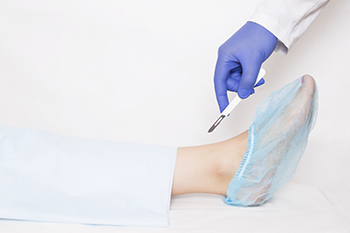
Ankle replacement surgery, or ankle arthroplasty, is a surgical option for those with severe ankle joint damage, often resulting from osteoarthritis, rheumatoid arthritis, or significant fractures. This procedure involves replacing the damaged bones in the ankle joint with prosthetics, to restore function and reduce pain. Ankle replacement surgery includes making an incision to access the joint, repositioning blood vessels, nerves, and tendons, and then removing and reshaping the damaged bones to fit the artificial joint. Full recovery may take as long as six months. It begins by keeping the leg elevated and possibly remaining in the hospital for up to a week, as the healing process begins. Though the prognosis is generally positive, with many ankle replacements lasting over a decade, potential risks can include infection, blood clots, nerve damage, and prosthetic failure. If you have severe ankle problems, it is suggested that you schedule an appointment with a podiatrist to find out if ankle replacement is an option for you.
In certain cases, in which the patient suffers from extreme pain or damage in a joint, joint replacement surgery may be deemed useful. If you have constant pain in a foot joint, consult with Dr. Odin De Los Reyes from Connecticut. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Joint Replacement Surgery?
Over time, joints wear down; this can be exacerbated by diseases and conditions. Joint replacement surgery, also known as arthroplasty, is when a damaged joint is surgically removed and replaced with a prosthesis. Prostheses, which can be made of ceramic, plastic, or metal, act as joints in lieu of an actual joint. One of the most prevalent causes for joint replacement is arthritis.
Arthritis in the Foot
Arthritis can occur in any joint in the body, including in the feet. Common types of arthritis in the foot are osteoarthritis, rheumatoid arthritis, and gout. The big toe is usually where arthritis occurs in the foot; this is known as hallux rigidus.
Joint Replacement Surgery in the Foot
The most common form of joint replacement in the foot is a first metatarsophalangeal (MTP) joint placement. MTP joint replacement surgery is designed to treat hallux rigidus. Surgery is not intensive, and recovery occurs within one to two months after the procedure has been done. Overall, joint replacement surgery is a safe and effective way to treat pain in the joint of the foot.
If you have any questions, please feel free to contact our offices located in Southbury and Farmington, CT . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Joint Replacement Surgery
When conservative, noninvasive treatments prove unsuccessful, podiatrists will often turn to surgery as the last line of treatment for their patients. If patients are suffering from joint pain, issues in mobility, or are seeking to correct a deformity, joint replacement surgery is an effective option. Joint replacement surgery is also successful in treating arthritis, which is the most common cause of improperly working joints.
Patients with symptoms that include joint pain, stiffness, limping, muscle weakness, limited motion, and swelling are typically considered for joint replacement surgery. Range of motion and activity post-surgery will vary between patients and depending on the specific surgery performed, the affected joint, and the damage that will need to be repaired.
Joint replacement surgery replaces the damaged cartilage and bone, the latter if required. The damaged cartilage is typically replaced with a prosthesis that is attached to the bone, allowing the implant to grow into the bone. Following surgery, the patient will typically undergo physical therapy to become familiar with movement using the replaced joint.
Types of Broken Toes and Relief Options
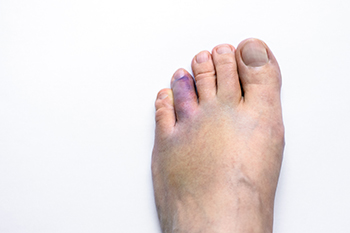
Diagnosing a broken toe involves recognizing symptoms such as intense pain, swelling, bruising, and difficulty walking. Types of toe fractures include stress fractures, where small cracks form from repetitive stress, and traumatic fractures, resulting from a direct blow or impact. A doctor will perform a physical examination and may order X-rays to confirm the diagnosis and determine the fracture type. Relief options for a broken toe include rest and elevation to reduce swelling and pain. Depending on the type of fracture, buddy-taping the injured toe to an adjacent toe may provide support and alignment during healing. Wearing stiff-soled shoes can protect the toe and ease walking. In severe cases, a cast or surgery may be necessary to ensure proper healing. If you have fractured your toe, it is suggested that you consult a podiatrist who can guide you toward a comprehensive treatment plan.
Broken toes may cause a lot of pain and should be treated as soon as possible. If you have any concerns about your feet, contact Dr. Odin De Los Reyes from Connecticut. Our doctor will treat your foot and ankle needs.
What Is a Broken Toe?
A broken toe occurs when one or more of the toe bones of the foot are broken after an injury. Injuries such as stubbing your toe or dropping a heavy object on it may cause a toe fracture.
Symptoms of a Broken Toe
- Swelling
- Pain (with/without wearing shoes)
- Stiffness
- Nail Injury
Although the injured toe should be monitored daily, it is especially important to have a podiatrist look at your toe if you have severe symptoms. Some of these symptoms include worsening or new pain that is not relieved with medication, sores, redness, or open wounds near the toe.
If you have any questions, please feel free to contact our offices located in Southbury and Farmington, CT . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What to Know About a Broken Toe
Trauma to the foot, especially the toes, can occur in many ways. Banging them, stubbing them, or dropping something on them are a few different ways this trauma can occur. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break or fracture. Another type of trauma that can break a toe is repeated activity that places stress on the toe for prolonged periods of time.
Broken toes can be categorized as either minor or severe fractures. Symptoms of minor toe fractures include throbbing pain, swelling, bruising on the skin and toenail, and the inability to move the toe with ease. Severe toe fractures require medical attention and are indicated when the broken toe appears crooked or disfigured, when there is tingling or numbness in the toe, or when there is an open, bleeding wound present on the toe.
Generally, a minor toe break will heal without long-term complications. However, it is important to discontinue activities that put pressure on the toe. It is best to stay off of the injured toe and immediately get a splint or cast to prevent any more additional movement of the toe bones. You can also immobilize your toe by placing a small cotton ball between the injured toe and the toe beside it. Then, tape the two toes together with medical tape. Swelling can be alleviated by placing an ice pack on the broken toe directly as well as elevating your feet above your head.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery, especially when the big toe has been broken. Due to its position and the pressure the big toe endures with daily activity, future complications can occur if it is not properly treated. Pain associated with minor toe fractures can be managed with over-the-counter pain medications. Prescription pain killers may be necessary for severe toe fractures.
The healing time for a broken toe is approximately four to six weeks. In severe cases where the toe becomes infected or requires surgery, healing time can take up to eight weeks or more. While complications associated with a broken toe are immediately apparent, it is important to note that there are rare cases when additional complications, such as osteoarthritis, can develop over time. You should immediately speak with your podiatrist if you think you have broken your toe due to trauma. They will be able to diagnose the injury and recommend the appropriate treatment options.
Benefits of Air Casts for a Broken Foot
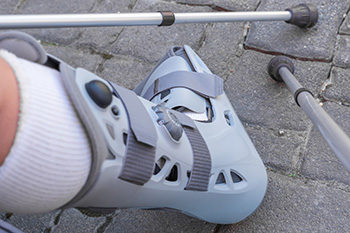
When facing a foot, ankle, or lower leg injury, patients often choose between a traditional hard cast and a modern air cast boot. An air cast boot, which encases the injured area in an air cushion within a hard plastic shell, offers several notable benefits. Primarily, it provides both stability and mobility. The adjustable air cells within the boot can be tailored for optimal comfort and support, reducing the risk of swelling. The boot's design also allows for limited movement, encouraging gradual weight-bearing and strength recovery. Unlike hard casts, air casts can be removed, which makes activities like showering easier. Additionally, the hard shell provides protection against impact, while the non-skid sole provides safety and stability. Air cast boots are versatile, suitable for minor injuries, and can be used as transitional support after a hard cast is removed. They are lightweight, customizable, and affordable. If you have a broken foot or ankle injury, it is suggested that you schedule an appointment with a podiatrist to see if an air cast is right for you.
A broken foot requires immediate medical attention and treatment. If you need your feet checked, contact Dr. Odin De Los Reyes from Connecticut. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Foot Causes, Symptoms, and Treatment
A broken foot is caused by one of the bones in the foot typically breaking when bended, crushed, or stretched beyond its natural capabilities. Usually the location of the fracture indicates how the break occurred, whether it was through an object, fall, or any other type of injury.
Common Symptoms of Broken Feet:
- Bruising
- Pain
- Redness
- Swelling
- Blue in color
- Numbness
- Cold
- Misshapen
- Cuts
- Deformities
Those that suspect they have a broken foot shoot seek urgent medical attention where a medical professional could diagnose the severity.
Treatment for broken bones varies depending on the cause, severity and location. Some will require the use of splints, casts or crutches while others could even involve surgery to repair the broken bones. Personal care includes the use of ice and keeping the foot stabilized and elevated.
If you have any questions please feel free to contact our offices located in Southbury and Farmington, CT . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.